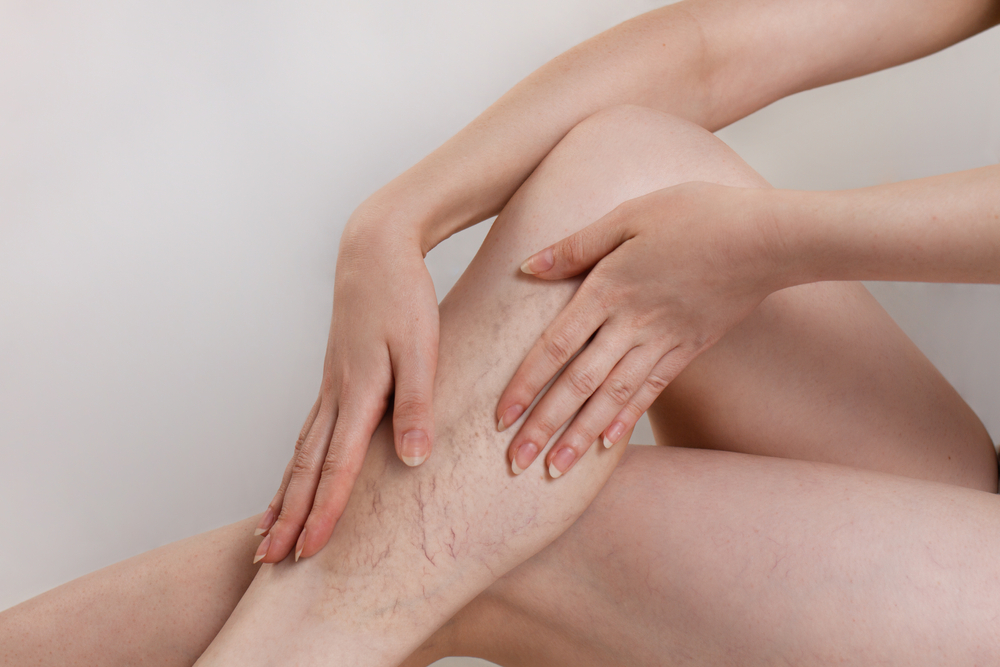
Countless people experience leaky veins in their legs, especially as they get older or through certain seasons of life. Perhaps you inherited vein-related issues from your parents or are dealing with the residual effects of an old injury. Either way, if you’re living with symptoms of leaky veins in your legs, you’re not alone — and there are many things you can do about it.
Unveiling the Structure: Anatomy of Vein Valves
To understand how veins can become leaky (and why this is problematic), we first need to review some anatomy. Interspersed throughout your veins are small crescent-shaped flaps of tissue, known as valves, that help prevent a backflow of blood. These valves project from the innermost layer of the vein wall to the center of the vein and are angled towards the heart in the direction of venous blood flow.
So, what is the function of valves in the veins? Valves in veins are like tiny doors that help blood travel back to your heart. These doors are made of special cells and tissue and work by opening when blood needs to go up toward your heart and closing to stop it from flowing back down.
This keeps the blood moving in the right direction and prevents it from pooling in your legs. If these valves don’t work properly, it can cause problems with circulation, leading to swollen legs or varicose veins.
What Are Leaky Veins In The Legs?
Leaky veins in the legs, also known as venous insufficiency, occur when the vein valves aren’t working properly. This causes blood to flow backward and pool in the legs.
Normal healthy valves act as one-way doors, so blood flows upward toward the heart and is unable to come back down. However, if these valves are damaged or weakened, they no longer close properly. This causes blood to leak back in the other direction, which is typically felt as increased pressure in the legs.
Symptoms and Diagnosis of Vein Valve Malfunctions
When you have a vein valve malfunction that’s causing leaky veins, you might experience a number of symptoms, such as[1]:
- Swelling in the legs, ankles, or feet
- Aching or throbbing sensations in the legs
- Feeling of heaviness or tiredness in the legs
- Visible varicose veins or spider veins
- Itching or burning sensations in the legs
- Skin discoloration, such as redness or brownish patches
- Leg cramps, especially at night
- Restless legs syndrome, which can make it harder to sleep or relax
- Ulcers or sores on the legs, particularly around the ankles
- Changes in skin texture, such as dryness or thickening
The severity and frequency of symptoms can vary. While some people have mild symptoms, others have vein problems that are indicative of more serious vein disease.
What Causes Vein Valves to Become Damaged?
Leaky veins can be caused by genetics, age, obesity, pregnancy, or prolonged standing or sitting. Let’s explore some of the common causes of damaged vein valves[1][2]:
The Aging Process
Vein walls weaken and expand as we get older, and the valve flaps may no longer reach each other in the closed position, allowing leakage.
Weak Valves
Vein valves are made of a protein called collagen. The characteristics of collagen vary slightly from person to person. Some people produce more flexible collagen, but others produce a relatively stiffer version that may make you more susceptible to damage.
Lack of Physical Activity
Muscular activity is important for healthy veins. As you contract your leg muscles, they gently compress the veins and assist the movement of blood through them. Having a desk or standing job that requires you to be sedentary for hours at a time reduces the beneficial effects of muscle activity and, as a result, blood flow becomes sluggish. Over time, this leads to venous hypertension, causing the veins to expand and the valves to become leaky.
Female Hormones
The female hormone progesterone softens the walls of the veins and the valve tissue. High levels of progesterone, as during pregnancy, can cause veins to expand and the valves to become leaky. Too much progesterone can also make the valves overly flexible and fail to close properly.
Estrogen, another predominantly female hormone, protects valves from damage through its anti-inflammatory characteristics. When vein circulation worsens, the number of estrogen receptors in the veins also increases — for both women and men.
Blood Clots
Valve damage can occur from a blood clot that develops in the leg, impairing blood flow. As backpressure builds, the valve eventually gives way and opens in the wrong direction, sustaining damage in the process. Additionally, if a blood clot forms on a valve, it can cause scarring that prevents the valve from opening and closing properly.
Accidents, Injuries, or Illness
Less commonly, a past accident or injury to the legs, surgery involving the legs, or a disease process that affects the circulation can also damage venous valves.
How are Damaged Vein Valves and Venous Insufficiency Treated?
Managing leaky valves in veins often first involves lifestyle changes, including simple self-care techniques you can incorporate into your routine to help with discomfort and improve blood flow.
Optimal Nutrition
Eating well isn’t just important for overall wellness, but also for healthy veins. Nutrients like vitamin E, vitamin B complex, copper, vitamin C, and vitamin K all play unique roles in vein health. The best way to ensure you’re getting a variety of important nutrients is to maintain a balanced diet that includes vegetables, fruits, nuts, seeds, whole grains, legumes, and lean proteins.
Compression Stockings
One useful option is compression stockings, which help prevent blood from pooling and can reduce swelling and achiness. These are available over-the-counter or by prescription if you need higher levels of compression. These can be worn anytime but are especially recommended during activities that worsen your symptoms, like sitting or standing for prolonged periods.
Physical Activity
Movement is key for overall health and the health of your veins. This can be as simple as walking, which gets blood flowing in your legs and can help reduce swelling and feelings of heaviness. For more health benefits, rotate in other activities, like swimming, playing tennis, bicycling, or doing an aerobics class.
Rest and Elevation
When you’re not exercising or doing other work, it’s essential to rest your legs in a way that helps reduce blood pooling and swelling. Elevate your legs above the level of your heart. For example, you might lie on the couch with your legs up on the arm or on a stack of pillows a couple of times daily.
Navigating Your Vein Health: When to See a Specialist
If you’re experiencing symptoms of leaky veins that aren’t well-managed by home techniques or are otherwise concerned about your vein health, it’s always best to get in touch with a specialist.
In some cases, medical intervention can be your best option for long-term symptom alleviation and improved blood flow. Minimally invasive vein procedures can be done to repair or remove the affected veins.
At Empire Vein & Vascular Specialists, we perform vein procedures in the comfort of our office, only requiring local anesthesia, including:
- VenaSeal™: A permanent solution for varicose veins that works by injection of a medical-grade adhesive that closes off the affected veins, and the blood is then rerouted to healthy veins.
- ClosureFast™: A solution that uses patented radiofrequency ablation (microwaves) to deliver uniform heat to treat and close affected veins and the blood is then rerouted to healthy veins.
- Sclerotherapy: A treatment for spider veins where an injection of a liquid compound is introduced directly into the veins that cause the veins to become absorbed by the body and the blood is then rerouted to healthy veins.
To learn more about vein valves and these treatments, schedule a free consultation at Empire Vein & Vascular Specialists. We’re the top provider of VenaSeal™, the leading outpatient varicose vein treatment in the USA.
To schedule a free consultation with our team of board-certified vascular surgeons, please call 1-800-827-4267 today.
References
- Patel SK, Surowiec SM. Venous Insufficiency. [Updated 2023 Jul 18]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430975/
- Ortega MA, Fraile-Martínez O, García-Montero C, et al. Understanding Chronic Venous Disease: A Critical Overview of Its Pathophysiology and Medical Management. J Clin Med. 2021;10(15):3239. Published 2021 Jul 22. doi:10.3390/jcm10153239
- Serra R, Gallelli L, Perri P, et al. Estrogen Receptors and Chronic Venous Disease. Eur J Vasc Endovasc Surg. 2016;52(1):114-118. doi:10.1016/j.ejvs.2016.04.020